A complex skin disease that began small
What you need to know:
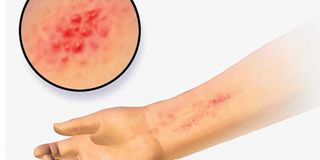
- She was busy scratching her body. Her skin; which had already lost most of the outer layer was peeling off. I noticed ulcers all over her body.
- Then I learnt another sad story about her—that for many years, the girl’s case had bewildered relatives and the health workers alike—it was a rare skin disease.
Recently, during my routine ward rounds at Benjamin Mkapa Hospital in Dodoma Region, one patient, a girl aged 20 captured my attention.
She was busy scratching her body. Her skin; which had already lost most of the outer layer was peeling off. I noticed ulcers all over her body.
Then I learnt another sad story about her—that for many years, the girl’s case had bewildered relatives and the health workers alike—it was a rare skin disease.
I learnt that the girl had actually been diagnosed with the condition, known in the doctors’ language as ‘mycosis fungoides’ (MF) at Kilimanjaro Christian Medical Centre (KCMC) in Moshi District before my observation. The disease is also known as Alibert-Basin- Syndrome.
As the girl narrated the story of her agony with the disease, she recalled the first day when she noticed rashes on her skin.
She says, “The rashes were itching severely.” She described the rashes in Kiswahili as, “Vilikuwa kama vipele vya baridi lakini vilikuwa vinawasha sana.’’ This means that the painful rashes appeared like they had been induced by cold weather. The problem started slowly as the girl narrates, “I had been experiencing dry itchy skin patches and I was being prescribed a lot of skin creams. I have been to many hospitals, including Muhimbili in Dar es Salaam,” she told me as I listened patiently.
The girl who, otherwise should have been attractive in appearance, was now looking so strange to me—something that even made her mother who accompanied her, sad.
The mother narrated to me that the girl’s situation had been getting worse, especially after she had stopped using medication. “Now, is she going to get over it?” she asked me, anxiously.
Why she stopped medication
Her mother recalls that at KCMC, cancer specialists had prescribed chemotherapy for the girl; and she had got 5 cycles of treatment.
I learnt that in the process, the experts at KCMC did their best to help the girl get out of the situation, especially during the initial stages.
By that time, the disease could not respond to common skin medication. That’s when the doctors arrived at the decision to put the girl on chemotherapy.
And, you know how expensive chemotherapy can be in Tanzania but thank God, she was on health insurance as a dependent member.
But on the other hand, being on health insurance couldn’t have saved the matter because there was this challenging issue, the cost of the drugs.
Initially, the cost was pegged at Sh600, 000 as per cycle of treatment. Now, was this exorbitant or not? Possibly not; because the next round of treatment was much more expensive.
Yet, as you may know, there is a long chain of steps to follow until the meds are brought on the table.
What’s done is that a doctor—and not just a doctor—a specialist had to write a letter to her insurance company before the drugs could be approved.
Even so, the drugs could not provide the expected cure to the girl’s problem.
When she was into her 4th cycle, the condition recurred.
This is when the oncologist at KCMC thought of something else—now believing that the condition was not one to be fully controlled by administering chemotherapy.
But in the girl’s version of the story, as she narrated to me recently, she said, “I got 5 cycles. I didn’t get the next cycles. I had been put on health insurance through my grandpa’s card. So, I was told that I am not eligible to get the medication. So, I have discontinued with medication for the past three months. That’s why I have come to Dodoma.”
“My condition is getting worse, that’s why I am here at the hospital for help. My skin is peeling off,’’ she appealed for help.
Here, an oncologist at Benjamin Mkapa Hospital in Dodoma, Dr Caroline Mrema, had to zero-in to sort the girl’s problem.
She devoted her time to the patient—visiting her from time to time and giving her the care she deserved. The doc now prescribed other medication. But, did the girl get them?
Look here, she was now supposed to travel all the way to Dar es Salaam to get them.
And, what are those medication? It’s those that are hard for a layperson to pronounce—the Ifosfamide, MESNA, Carboplatin, Etoposide and G-CSF. By the way, they are more expensive than the previous ones that she had been given at KCMC.
Given, that she had a problem with her health insurance, it was now becoming clear that she had to go through another round of hustles to get the treatment she deserved.
Revealing the condition
As for me, the fact remained—that I was seeing such a case of MF for the first time. How does it occur? To understand it well, you need to know what we call T-cells. These cells are like policemen.
They are special type of white blood cells which regulate the body’s defense system and their job is to fight infections.
Now, the theory is that these cells could become cancerous. That’s why doctors say MF is a T-cell Lymphoma—a slowly growing form of cancer in which some of the body’s white blood cells turn cancerous. What happens is that these abnormal cells are drawn to the skin and some are deposited there.
The challenging thing is that doctors usually misdiagnose and treat it as a common skin condition known as eczema.
Recently, Dr Mrema unraveled to me some important facts about this disease.
She explained to me the tribulations that patients with MF go through. She said, “The disease is very rare…and I must admit that it’s my first time to meet with an MF victim with advanced severe skin damage.”
She added, “The slow growing form is hard to cure with chemotherapy.”
Then she leaped into what I eagerly wanted to hear, she said, “The worrying thing is that, the real cause is unknown, it is neither contagious nor hereditary in most cases.”
“In the early stages, it’s usually treated by skin specialists (dermatologist) but in advanced stage, it should be treated in centers specialising on such conditions,” Dr Mrema added.
Dr Lugano is a medical doctor now based in Dodoma.




