One step at a time as Tanzania fights lifestyle diseases
What you need to know:
- In 2010, the World Health Organisation (WHO) released a report titled, ‘Global status report on non-communicable diseases: Description of the global burden of NCDs, their risk factors and determinants that stated that the diseases were affecting 47 per cent of patients and that, out of the 100 that died, 60 died of NCDs.
Tanzania is among the developing countries facing the major challenge of Non-Communicable Diseases (NCDs).
Despite efforts being made by health stakeholders in fighting the diseases, more is yet to be done.
In an exclusive interview, The Citizen’s reporter Herieth Makwetta speaks to the minister for Health, Community Development, Gender, the Elderly and Children, Ms Ummy Mwalimu, who explains what the government is doing to implement strategies and policies aimed at countering the diseases.
What does it mean when we speak of NCDs and how has Tanzania repositioned itself in countering them?
In 2010, the World Health Organisation (WHO) released a report titled, ‘Global status report on non-communicable diseases: Description of the global burden of NCDs, their risk factors and determinants that stated that the diseases were affecting 47 per cent of patients and that, out of the 100 that died, 60 died of NCDs.
These statistics show that if concerted action is not taken to fight the diseases by 2020, the statistics will go up from 47 to 60 per cent and the death rate will also shoot up from 60 to 73 per cent.
Here in the country, we get a picture about NCDs through a study conducted in Dar es Salaam, Mara and Kilimanjaro regions in the 1990s, but I would not like speak about that as for now we are using a study carried out in 2012 by the National Institute for Medical Research (Nimr).
Nimr carried out the study in collaboration with the WHO, the Ministry of Health and health stakeholders as it is the one that we have been using to date, giving us a summary on NCDs.
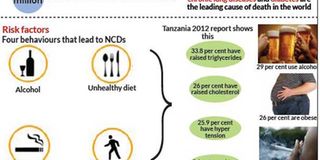
The findings of the research show that 15.9 per cent of Tanzanians use tobacco and this includes cigarette smokers that are a catalyst for respiratory diseases, 29 per cent are alcohol drinkers that are considered one of the main causes of the diseases, 26 per cent are obese and overweight, 26 per cent have raised cholesterol in their body and 33.8 per cent have raised triglycerides, the main constituents of natural fats and oils.
The findings of the study also show that 9.1 per cent are diabetic while 25.9 per cent suffer from hypertension.
The government launched a campaign called ‘Afya yako, mtaji wako’ that sensitised people to engage in physical exercises so as to fight NCDs. Has the campaign brought about positive results?
The campaign was a result of the study carried out in 2012, whereby a quarter of interviewees said they were neither exercising nor doing laborious jobs. Out of those interviewed, four said they neither engaged in any physical exercises nor did any physical work and this gave us a picture of NCDs in the country.
I admit that the campaign has not succeeded to its full potential in the implementation of the exercise campaign.
I must be realistic that we started well, but our expectations were that every council would have continued with the implementation of the campaign that was launched by Vice President Samia Suluhu Hassan.
We met with council and discussed together that there was a need of relaunching the campaign that was being implemented in some regions.
Is there any current policy or guidelines for fighting NCDs currently?
In 2016, the government designed and launched a five-year national strategy for fighting NCDs. The strategy has already identified the areas that we will work on.
Tobacco consumption is one major risk factor for NCDs. What is the government doing on tobacco control?
Tanzania is a member of WHO as we have signed the 2007 framework convention on tobacco control.
I must admit that the framework is outdated as there are some areas that have not been worked upon, despite the fact that we have managed to control tobacco smoking in some areas, particularly airports, where there were no warnings on smoking. We have gone as far as special rooms for smoking. The challenge we face is on open space areas.
That has not been tackled as the law requires people not to smoke in those open space areas, but there has been confusion about who is supposed to enforce the law, it is a policeman or a health officer? The law confuses and that is why before I became the health minister, efforts were made to amend the law on tobacco control and a new one was introduced.
However, we need to agree that the new law is on the issue of controlling tobacco farming. For instance, if you tell tobacco farmers in Urambo and Tabora rural not to cultivate the crop that is part of increasing their incomes, I don’t think they will understand you.
What we need now is to discuss the matter within the government while tobacco stakeholders need to come up with alternative farm crops that will help increase their incomes.
The alternative farm crops will not affect their incomes and even their future lives.
Besides that, what efforts are being made?
I’m very happy to hear that question as two weeks ago a meeting was called by the Prime Minister’s Office that the time had come to agree with one another on how we can have a common stand as a country and as a government in controlling the use of tobacco.
However, we as a Ministry of Health have said that since there is no law and the one existing is outdated, we will neither ban nor go against tobacco farming.
We will educate members of the public about the effects of tobacco use. That is our main objective.
To avoid spending huge sums of cash on treating the diseases, what is the government doing on prevention?
Even in the 65th conference of health ministers from East, Central and Southern Africa, we discussed that the main risk factors of NCDs is the use of tobacco and excessive alcohol consumption.
Also the issue of a life style was highlighted as many people don’t walk long distances. All these risk factors are worked upon.
Do we have a recent study on NCDs?
A special study was conducted in 2012, almost six years ago, but when you look at the number of patients going to health centres due to NCDs have been increasing.
Now, what’s the next plan as we look ahead?
We have repositioned ourselves in three big areas: first on prevention, second on early diagnosis and third on medical treatment.
Currently, we are focused on preventing people from falling a victim to NCDs by educating them through awareness programs.
As part of low-cost interventions, WHO recommended a minimum amount of money that should be allotted to every Tanzanian in fighting NCDs? If so, is it sufficient?
What we get is a budgeted disbursement from the Central Government.
But, we need to find ways of improving the funding. For instance, in South Africa sugar is taxed because of its massive use and it is a contributing factor to NCDs and eventually contributes to medical care bills, hence sugar is taxed.




